Contents

How bad is bladder cancer?
· From a bladder cancer to kidney failure. Makram Khalife, a 71-year-old retired bank manager from Lebanon, shares how bladder cancer led to his kidney function declining and ultimately the removal of one of his kidneys. … BCG is a germ that’s related to the one that causes tuberculosis (TB).] I received this treatment three times a month for …
What is the main cause of bladder cancer?
Can Bladder Cancer Be Cause Chronic Kidney Disease. A large number of Americans are thought to suffer from chronic Kidney Disease. The majority of the time dialysis or kidney transplants are the only choices for those in the advanced stages of the disease. Get to the Kidney Disease Solution, an all-in-one resource to improve kidney health and function.
What are the risks of bladder cancer?
· An obstruction blocking the ureter connecting the kidney to the bladder can increase the risk of kidney failure. When bladder cancer is detected at this early stage, the first-line treatment is a transurethral resection (TUR), which removes the cancerous cells and preserves the function of the bladder.
How does bladder cancer affect the urinary system?
· Having bladder cancer may also be related to the increased risk of kidney cancer. It may also increase the risk of the following other cancers: A second bladder cancer that is dissimilar than the first cancer coming back. Another primary cancer in the ureter, renal pelvis, pancreas, larynx, lung, prostate, or female genital organ.

What type of cancer causes kidney failure?
Kidney failure and damage are common complications of multiple myeloma, a type of blood cancer.
What organs are affected by bladder cancer?
You get bladder cancer when bladder cells become abnormal and grow out of control. Over time, a tumor forms. It can spread to nearby lymph nodes and other organs. In severe cases, it can spread to distant parts of your body, including your bones, lungs, or liver.
Is kidney failure common in cancer patients?
Because CKD, defined by an estimated glomerular filtration rate (eGFR) < 60 ml. min/1.73 m2, is common, with a prevalence of about 4% in the adult population aged 20 years and older, reaching 30% or more in the elderly, it is expected to be also common in patients with any type of cancer.
What happens in the final stages of bladder cancer?
When bladder cancer reaches stage 4, the original tumor has often grown and pushed through the wall of the bladder. Cancer cells may have spread to organs close to the bladder or those further away, such as the liver or lungs.
What can bladder cancer lead to?
Chronic bladder infections and irritation: Problems associated with increased bladder cancer risks include urinary infections, kidney and bladder stones, and other causes of bladder irritation.
What are the symptoms of advanced bladder cancer?
Symptoms of Advanced Bladder CancerAn inability to urinate.Lower back pain on one side of the body.Loss of appetite.Unintended weight loss.Overwhelming fatigue.Bone pain.Swelling in the feet.
What happens when a cancer patients kidneys fail?
Acute renal failure (ARF) is defined as a sudden decrease in glomerular filtration rate leading to an acute rise in blood urea nitrogen and serum creatinine levels. It is a serious complication of cancer and constitutes a major source of morbidity and mortality.
How does cancer affect kidneys?
Kidney cancer develops when cells in your kidneys change and grow out of control. People with kidney cancer may notice flank pain, high blood pressure, blood in their pee and other symptoms. Kidney cancer treatments include surgery, chemotherapy and radiation therapy.
Is kidney failure worse than cancer?
Kidney disease, also known as chronic kidney disease or CKD, causes more deaths than breast cancer or prostate cancer (NVS 2021 report of 2018 data).
Where does bladder cancer usually spread to?
Not all bladder cancers will spread. But If it does it’s most likely to spread to the structures close to the bladder, such as the ureters, urethra, prostate, vagina, or into the pelvis.
What are the symptoms of late stage bladder cancer?
Symptoms of advanced bladder cancerBeing unable to urinate.Lower back pain on one side.Loss of appetite and weight loss.Feeling tired or weak.Swelling in the feet.Bone pain.
How long do you have to live with Stage 4 bladder cancer?
The 5-year survival rate is the rate of surviving for 5 years after a cancer diagnosis. For bladder cancer, if the cancer has spread to the regional lymph nodes, the 5-year survival rate is 36.3 percent . If it has spread to a more distant site, the 5-year survival rate is 4.6 percent .
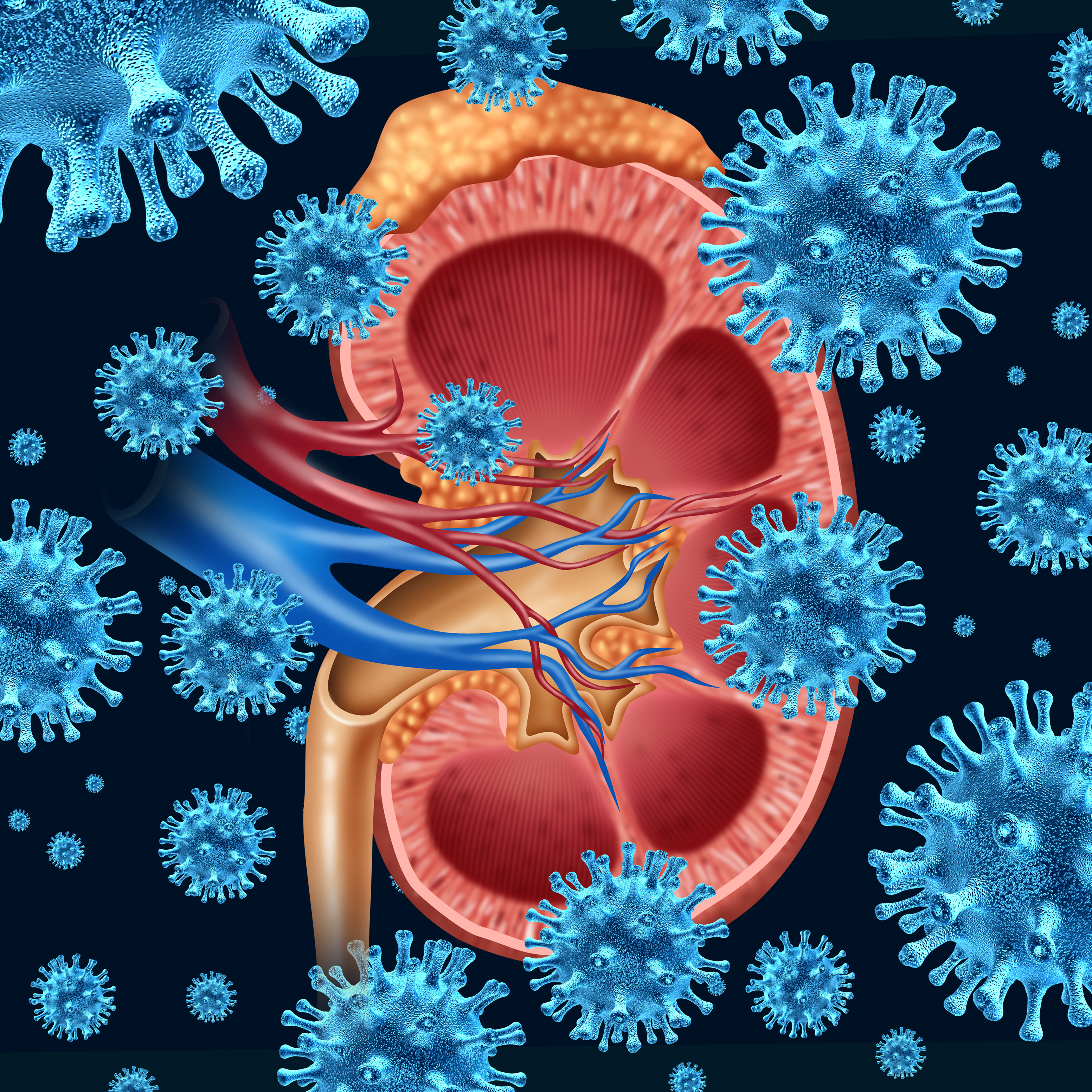
What is the function of bladder?
Bladder is balloon-shaped urine storage. It temporary stores urine from the kidney before eventually you empty the bladder when you pee. Together with kidneys, it plays a key role in your urinary system – see the following image (image credit to Cancer Research UK).
What are the risk factors for kidney cancer?
But experts have confirmed the risk factors of the disease are as follows: Older age, the risk to have the disease increases with age. Cigarette smoking. Kidney disease, especially if it requires kidney dialysis.
What are the second cancers?
Other second cancers that may occur include: A second kidney cancer, and this is different than the first cancer recurring. Another primary cancer in the thyroid, ureter (tube that carries urine from the kidney to the bladder), or prostate. Melanoma of the skin.

What is secondary kidney cancer?
Kidney cancer. It is a type of cancer that develops from cells of the kidney. Cancer elsewhere in the body can also spread to the kidney and this is called secondary cancer, not primary kidney cancer because it acts like the cancer in the original organ where it first started.
What is it called when you have a second cancer?
When people with a cancer develop another new, unrelated cancer – it is called a second cancer. For instance, a few people with primary prostate cancer may also develop another primary cancer in the bladder – even after surviving the first. Sometimes a new cancer may also occur in the same organ as the first.
What are the first degree relatives of kidney cancer?
First degree relatives include parent, brother, and sister. People with healthy weight are at lower risk than obese people. Some medications such as particular painkillers or treatment for another cancer. In addition, there are a number of different types of kidney cancer.

What are the inherited diseases that affect the kidneys?
Particular inherited conditions and faulty genes affecting the kidneys such as tuberous sclerosis and Birt-Hogg-Dubé syndrome. Hypertension, high blood pressure. A family history, especially first degree relatives, of kidney cancer.
How to treat bladder cancer?
Treatment of Bladder Cancer 1 Removal during cystoscopy 2 Intravesical immunotherapy or chemotherapy (for superficial, or surface, cancers) 3 Partial or total removal of the bladder, radiation, chemotherapy or immunotherapy (for deeper, more invasive cancers)
What is the tube that is inserted into the bladder to see blood?
Videos (3) Bladder cancer most often causes blood in the urine. To make the diagnosis, a thin, flexible viewing tube (cystoscope) is inserted through the urethra into the bladder. Many cancers are treated with removal, using a cystoscope (for surface cancers) or by removing the bladder (for deeper cancers).

What is needed to determine if bladder cancer has spread?
The urethra is anesthetized somewhat so the procedure is not too uncomfortable. If the cancer has invaded the bladder muscle, additional testing, including abdominal CT and chest x-ray, is needed to determine whether a cancer has spread.
How does the neobladder work?
For an orthotopic neobladder, the reservoir is connected to the urethra. The person learns to empty this reservoir by relaxing the pelvic floor muscles and increasing pressure within the abdomen, so that urine passes through the urethra very much as it would naturally. Most people are dry during the day, but some urine leakage may occur at night.
How to drain urine from a person?
The usual way has been to route the urine to an opening (stoma) made in the abdominal wall through a passageway made of intestine, called an ileal loop. The urine is then collected in a bag worn on the outside of the body.

What type of cell is bladder cancer?
VIDEO. Most bladder cancers are of a type called transitional cell, affecting the same kinds of cells (transitional cells) that are usually the cancerous cells responsible for cancers of the renal pelvis and ureters.
How many people die from bladder cancer in 2019?
According to 2019 estimates, more than 17,500 people die of bladder cancer every year. About 3 times as many men as women develop bladder cancer. Smoking is the greatest single risk factor and seems to be one of the causes in at least half of all new cases. Certain chemicals that are used in industry can become concentrated in …
What is the abbreviation for eGFR?
eGFR : estimated GFR with the abbreviated MDRD equation in ml/min/1.73 m2;
What is the most common cancer after transplant?
From the beginning of transplantation, a high incidence of lymphoma and skin cancers, was observed in graft recipients. (7) The skin is by far the most frequent site of malignancies after transplantation. Nonmelanoma skin tumors, including squamous cell and basal cell carcinomas, account for 95% of these skin cancers, whereas rare tumors such as melanoma and Kaposi’s sarcoma account for the other 5%.(50, 51) However, as graft and patient survival have improved due to better immunosuppressive agents, the risk for various other types of cancer has also increased. Because the incidence of most cancers is low, it is difficult to assess from a single center. Moreover, reporting of cancers to transplant registries is often incomplete and may lead to underestimate the risk. In the past five years, nevertheless, a few large studies have examined site-specific cancer risk for a wide spectrum of tumors by linking national transplant registry database with those of either national cancer registry (10, 11, 13, 14) or Medicare billing claims. (12) Four of them which identified at least 500 cancer cases are described in Table 1. (14) Two studies (13, 14) did not include nonmelanoma skin cancers, and tended to show lower overall risk than the others. (10–12) In US kidney transplant patients, the risk (cumulative incidence) of skin cancer (excluding melanoma) was 7.4 % at three years and that of any nonskin cancer (but including melanoma), 7.5%.(12) Cancer risk (excluding nonmelanoma skin cancer) has been estimated at 20% after 10 yrs of immunosuppression in Australia and New Zealand, (7) but lower in Canada, 12% after 17 yrs. (14)
How long after transplantation does bcumulative incidence increase?
bcumulative incidence at 3 yrs after transplantation (number of cancers not available)
Is CKD a risk factor for cancer?
In contrast with cancer risk associated with dialysis and transplantation, the potential of early stage CKD as a risk factor for cancer is not established. Concern arose recently, however, from a few large cohorts which studied cancer mortality or incidence in individuals with and without CKD, defined by their baseline estimated glomerular filtration rate (eGFR) or albuminuria level. (15–17) Fried et al (15) were the first to display an increase in cancer mortality associated with decreasing renal function in the elderly population from the Cardiovascular Health Study. Excess in mortality risk was limited to the highest vslowest quartile for cystatin C (>1.22 vs<0.93 mg/L) as well as to the lowest vshighest quartile for MDRD eGFR (<60 vs> 81 ml/min/1.73 m2) with adjusted hazard ratio (HR) of 1.79 (95% confidence interval: 1.33;2.42) and 1.30 (0.97;1.74), respectively. Because of the relatively small number of events, however, the authors were unable to adjust for other factors than age, gender, and race. These findings were confirmed and further investigated by Wong et al in the Blue Mountains Eye Study. (Table 1) (17) In this cohort, the authors observed an excess risk of cancer associated with moderate CKD, although it was limited to men.( Table 2) The excess risk began at an eGFR of 55 mL/min/1.73 m2, consistent with Fried et al’s findings, (15) and increased linearly as eGFR declined. Every 10 mL mL/min/1.73 m2was associated with a 29% increase of cancer risk independent of age and smoking, with the greatest risk at an eGFR < 40 mL/min/1.73 m2. The association seemed to be site specific for lung and urinary tract cancers. With a larger but younger cohort, Jorgensen also observed a 20% higher risk of all cancer with each standard deviation increase of albuminuria (log of albumin to creatinine ratio), and significant higher risks for lung, colon, kidney, and bladder cancers. (Tables 1and and2)2) Vajdic et al (13) examined the risk of cancer up to five years before starting renal replacement therapy in a cohort end-stage CKD patients. (Table 1) As expected, these patients were at higher risk for cancers known to cause ESRD such as kidney and bladder cancers and multiple myeloma, but they also showed excess risk for Kaposi sarcoma, non-Hodgkin lymphoma, and for cancers of the oral cavity, colon and thyroid. (Table 2) Immunologic alterations associated with CKD would be a likely cause for the excess of virus-related cancers, but explanations are lacking for the excess of thyroid cancer.
Is Ben a chronic disease?
BEN is a chronic tubulointerstitial nephritis with slow progression to ESRD and an increased incidence of upper urinary tract urothelial carcinoma. (45–47) It is endemic in several rural areas of the Balkans. BEN and acid aristolochic nephropathy are very similar with respect to both clinical and morphological aspects. That exposure to AA through consumption of flour contaminated with seeds of Aristolochia clematitis may be responsible for BEN in endemic areas is an old hypothesis. (46) The detection of AA-specific DNA adducts in renal tissue of a number of BEN patients and individuals living in endemic areas recently provided new evidence for a causal association. (48, 49)
Can analgesics cause urothelial cancer?
Toxins, such as analgesics and aristolochic acid, can induce both chronic interstitial nephritis and urothelial cancers. The association of analgesic nephropathy with the occurrence of urothelial carcinoma was first described in Sweden in 1965, and subsequently confirmed in several other countries. (27–32) Tumors were mainly transitional cell carcinomas located in the renal pelvis, the upper urinary tract and the bladder, but renal cell carcinomas were also described. (33) Phenacetin was recognized as the main culprit in both diseases and withdrawn from the market during the 1970s. In Australia, further evaluation of the effect of withdrawal of phenacetin-containing analgesics showed a significant decline in ESRD incidence due to analgesic nephropathy and a trend toward less renal pelvis and bladder cancers. (34, 35) Although the role of acetaminophen or other nonphenacetin analgesics in the occurrence of analgesic nephropathy is still debated, (36) neither of them has been convincingly linked with cancer. (37, 38)
How long after kidney transplant can you have dAge adjusted rate ratio?
dAge-adjusted rate ratio (n cases and CI not available) for cancer in women (except for prostate) 3 years after kidney transplantation

What is the most common cause of prostate cancer?
So far, prostate cancer has become popular among men above 50 years. It occurs as a result of uncontrolled growth of prostate glands that affects urinary system adversely. The mostly affected organs include urethra and the bladder and it may lead to kidney failure.
What causes kidney stones?
This leads to the accumulation of bacteria that spreads in the kidneys thereby subjecting them to failure. Kidney failure due to prostate cancer may lead to the formation of kidney stones.
What is the link between prostate cancer and kidney failure?
The Link Between Prostate Cancer And Kidneys Failure. Michael Wight. Prostate cancer occurs when the cells found in prostate glands grow uncontrollably. Prostate cancer kidney failure develops in men especially elderly ones. They are of different types and results to adverse effects on overall body health of the victim.

What are the most common conditions that affect elderly men?
This may bring many activities in the body to a standstill causing severe conditions or even death. Kidney stones and prostate cancer are the most common conditions that affect elderly men.
What is prostate removal?
which involves removal of the enlarged prostate glands safely without affecting other organs. This activity is carried out by an urologist. They further prescribe medications which should be taken as directed to promote quick recovery.
How to prevent kidney failure from prostate cancer?
This involves eating healthy and incorporation of exercise programs. These practices include:
Why is it important to treat prostate cancer early?
Early treatment of prostate cancer helps to prevent adverse conditions that can lead to chronic diseases or even death. Therefore, it is advisable to keep checking on the body for unusual changes. Those already in this mess can acquire treatments which help to restore their health.
What is the survival rate for cervical cancer?
According to the National Cancer Institute, the 5-year survival rate for cervical cancer that’s spread to regional lymph nodes is 58.2 percent. The 5-year survival rate for cervical cancer that’s spread to more distant tissues is 17.6 percent.
What is the treatment for kidney failure?
Kidney failure is often treated with dialysis, which helps to filter waste and excess fluids from your blood. If you have kidney failure with cervical cancer, your doctors will talk with you about your treatment options, including their risks and benefits.

What stage of cancer is kidney involvement?
Kidney involvement in cervical cancer is typically observed in advanced stages, specifically stages 3 and 4.
What is the purpose of a stent?
The stent helps to widen a narrowed ureter, allowing for urine to pass from the kidneys to the bladder.
How does hemodialysis work?
Hemodialysis. Hemodialysis uses a machine to move your blood through a filter that’s located outside your body. This filter works to remove waste and extra fluid from your blood. The filtered blood is then returned to your body.
Can cervical cancer cause kidney failure?
It’s also possible for cervical cancer to impact other areas of the body, such as the kidneys. Some individuals with advanced cervical cancer can go on to develop kidney failure.
Can cervical cancer spread to kidneys?
It’s also possible for cervical cancer to spread (metastasize) to the kidneys, potentially leading to kidney damage and failure . However, this is extremely rare. As of 2019, only 13 instances of kidney metastases had been reported in medical literature.
How many people have CKD?
CKD occurs in 29% of patients with kidney cancer and 46% of those with bladder cancer, according to the review. Individuals with end-stage kidney disease are particularly susceptible to malignancy, they stated. Patients on peritoneal dialysis appear to have a higher incidence of bladder and urinary tract cancer, hepatocellular carcinoma, …

Can CKD be caused by paraneoplastic glomerulopathy?
Paraneoplastic glomerulopathies, such as membranous nephropathy, IgA nephropathy, minimal change disease, membranoproliferative glomerulonephritis, and extracapillary glomerulonephritis can lead to CKD in patients with cancer. A subset of patients who undergo radical nephrectomy also later develop kidney disease.
Does ADT increase AKI?
Androgen deprivation therapy (ADT) used to treat prostate cancer may increase AKI risk, especially when luteinizing hormone-releasing hormone agonists are combined with antiandrogens, Dr Malyszko and her coauthors observed. Use of denosumab, a monoclonal antibody that treats skeletal metastases, may result in hypocalcemia.
Can chemo cause kidney failure?
Systemic chemotherapies can directly or indirectly harm the kidneys. Clinicians need to carefully monitor the dose and duration of use. Cisplatin, for example, can cause AKI in 20% to 30% of cases. Many other conventional agents also can contribute to nephrotoxicity. These agents include methotrexate, gemcitabine, mitomycin C, ifosfamide, pemetrexed, antimetabolites, and nitrosoureas.

Can cancer affect the kidney?
Nephrologists should be informed and actively involved in certain facets of cancer care, according to the authors. Cancer and its treatment may harm the kidney. Likewise, impaired renal function can complicate cancer management and worsen oncologic outcomes.
Does nivolumab cause kidney disease?
Immunomodulators and immunotherapy have been linked with adverse effects on the kidneys. Among immune checkpoint inhibitors, use of nivolumab, an anti-PDL-1 monoclonal antibody, can result in hypophosphatemia, proteinuria, and hypertension. Pembrolizumab, an anti-PD-1 monoclonal antibody, can cause acute interstitial nephritis and, rarely, AKI.
Can interleukin 2 cause capillary leak syndrome?
Recombinant human interleukin-2 (IL-2) can cause capillary leak syndrome with hypovolemia and AKI. Recombinant interferon-α (IFN-α) can induce proteinuria or even nephrotic syndrome.

What happens when your kidneys are unable to filter?
Acute kidney failure occurs when your kidneys suddenly become unable to filter waste products from your blood. When your kidneys lose their filtering ability, dangerous levels of wastes may accumulate, and your blood’s chemical makeup may get out of balance. Acute kidney failure — also called acute renal failure or acute kidney injury — develops …
What drugs can slow blood flow to the kidneys?
Diseases and conditions that may slow blood flow to the kidneys and lead to kidney injury include: Use of aspirin, ibuprofen (Advil, Motrin IB, others), naproxen sodium (Aleve, others) or related drugs.
What is the function of the glomeruli?
The glomeruli filter waste products and substances your body needs — such as sodium, phosphorus and po tassium — which then pass through tiny tubules. The substances your body needs are reabsorbed into your bloodstream. The waste products flow through the ureters — the tubes that lead to the bladder. Acute kidney failure occurs when your kidneys …

What diseases can cause kidney failure?
These diseases, conditions and agents may damage the kidneys and lead to acute kidney failure: Glomerulonephritis (gloe-mer-u-loe-nuh-FRY-tis), inflammation of the tiny filters in the kidneys (glomeruli) Hemolytic uremic syndrome, a condition that results from premature destruction of red blood cells.
What happens when you have kidney failure?
Acute kidney failure can occur when: You have a condition that slows blood flow to your kidneys. You experience direct damage to your kidneys. Your kidneys’ urine drainage tubes (ureters) become blocked and wastes can’t leave your body through your urine.
How to manage kidney disease?
Work with your doctor to manage kidney and other chronic conditions. If you have kidney disease or another condition that increases your risk of acute kidney failure, such as diabetes or high blood pressure, stay on track with treatment goals and follow your doctor’s recommendations to manage your condition.

How does blood enter the kidneys?
Blood enters your kidneys through your renal arteries. Your kidneys remove excess fluid and waste material from your blood through units called nephrons. Each nephron contains a filter (glomerulus) that has a network of tiny blood vessels called capillaries. The glomeruli filter waste products and substances your body needs — such as sodium, phosphorus and potassium — which then pass through tiny tubules. The substances your body needs are reabsorbed into your bloodstream. The waste products flow through the ureters — the tubes that lead to the bladder.