Contents
A notable new FDA approval in December 2019 was enfortumab vedotin (Padcev), approved for advanced bladder cancer patients who have not responded to chemotherapy or immune checkpoint drugs.
What is the most effective treatment for bladder cancer?
Chemotherapy followed by radical cystectomy (removal of the bladder and nearby lymph nodes) is then the standard treatment. Partial cystectomy is rarely an option for stage III cancers. Chemotherapy (chemo) before surgery (with or without radiation) can shrink the tumor, which may make surgery easier.
Are most bladder cancers curable?
What are the most common treatments for bladder cancer? Bladder cancer is highly treatable when it is diagnosed in the early stages.
What is the success rate of immunotherapy for bladder cancer?
Ultimately, what the study showed is that about 40 percent of patients can have their cancer eradicated with PD-1 immunotherapy, and about half of those responses last more a year.
Does bladder cancer ever go away?
This is very common if you’ve had cancer. For other people, bladder cancer might never go away completely or might come back in another part of the body. Some people may get regular treatment with chemotherapy , immunotherapy, or other treatments to try to keep the cancer in check.
Is a 5 cm bladder tumor large?
CONCLUSIONS: Larger tumor size (>5 cm) is associated with greater length of stay, reoperation, readmission, and death following TURBT. Patients should be counseled appropriately and likely warrant vigilant observation prior to and following hospital discharge.
Are most bladder cancers caught early?
Bladder cancer can often be found early because it causes blood in the urine or other urinary symptoms that cause a person to see a health care provider. In most cases, blood in the urine (called hematuria) is the first sign of bladder cancer.
What is the best hospital for bladder cancer?
Mayo Clinic in Rochester, Minn., Mayo Clinic in Phoenix/Scottsdale, Ariz., and Mayo Clinic in Jacksonville, Fla., have been ranked among the Best Hospitals for urology and cancer in the nation by U.S. News & World Report.
Can metastatic bladder cancer go into remission?
Bladder cancer is also sensitive to chemotherapy, and treatment for metastatic bladder cancer using methotrexate, vinblastine, doxorubicin, and cisplatin (MVAC chemotherapy) provides a response rate of 50%–70% and complete remission in 12%–40% of cases [27–30].
How long does immunotherapy last for bladder cancer?
These drugs are given as intravenous (IV) infusions, usually every 2 to 6 weeks, depending on the drug.
Can you live 10 years with bladder cancer?
Bladder cancer survival rates by stage According to the American Cancer Society , the relative survival rates for all stages of bladder cancer are: 5 years: 77 percent. 10 years: 70 percent. 15 years: 65 percent.
What foods should you avoid if you have bladder cancer?
However, avoid high intake of foods like red and processed meat, chewing areca nuts, consuming arsenic containing water, taking fried eggs and lifestyle factors such as smoking tobacco as it may increase the risk of bladder cancer, impact the prognosis and treatment outcomes, worsen symptoms, or increase the chances of …
What are the odds of beating bladder cancer?
5-year relative survival rates for bladder cancerSEER Stage5-year Relative Survival RateIn situ alone Localized96% 70%Regional38%Distant6%All SEER stages combined77%Mar 1, 2022

What percentage of bladder cancer is superficial?
Bladder Cancer Liver Gallbladder and Pancreas Urological Conditions Cancer. Over 75 percent of bladder cancers remain confined to the lining of the bladder and do not invade the bladder wall. These are called nonmuscle-invasive bladder cancer, or superficial bladder cancer, and when managed well, they are associated with excellent prognoses.
What is the drug that kills cancer cells?
Mitomycin C is a chemotherapy drug that kills the normal DNA function in cancer cells and is easily absorbed into the bloodstream through the bladder’s lining.
What is a cystoscope?
Cystoscopy is an outpatient procedure during which a thin, lighted tube with a camera is passed through the urethra into the bladder, allowing your doctor to see the inside of the bladder. Most modern cystoscopes are also equipped with channels that permit small instruments to be passed into the bladder.
How does chemotherapy work?
Chemotherapy uses chemical agents to interfere with replication and other normal functions of cells, resulting in tumor shrinkage or cancer cell death . The use of two or more chemotherapy drugs together has been found to be more effective than a single drug alone. There are several types of chemotherapy.
How often is urine syptoma emptied?
The urine is siphoned out of the urinary reservoir with a small catheter every four to six hours. The catheterizable pouch may require surgical repair at some point after surgery due to the wear and tear of frequent catheterization. This type of reconstruction is not performed on patients with a history of bowel disease.
Is immunotherapy better than chemotherapy?
There are a few FDA-approved immuno therapy drugs available for treating advanced and metastatic bladder cancer that has worsened after chemotherapy. Scientists are also investigating the possibility that combinations of immunotherapy drugs could be more effective than individual drugs.

Is bladder cancer non-invasive?
Bladder cancer treatment options vary depending on whether the cancer is nonmuscle-invasive or muscle-invasive, and specific treatments are determined based on the stage and grade of the tumor (s).
When will bladder cancer be treated?
New Treatments For Bladder Cancer in 2020. In 2019 and early 2020, the U.S. Food and Drug Administration (FDA) approved a number of new drugs for bladder cancer of all stages, and more treatments are on the horizon.
What is the FDA approved treatment for bladder cancer?
Advanced and metastatic bladder cancer treatment. A notable new FDA approval in December 2019 was enfortumab vedotin (Padcev), approved for advanced bladder cancer patients who have not responded to chemotherapy or immune checkpoint drugs. In clinical testing, this antibody-drug conjugate produced responses in 44% of patients who failed …

What is NMIBC treatment?
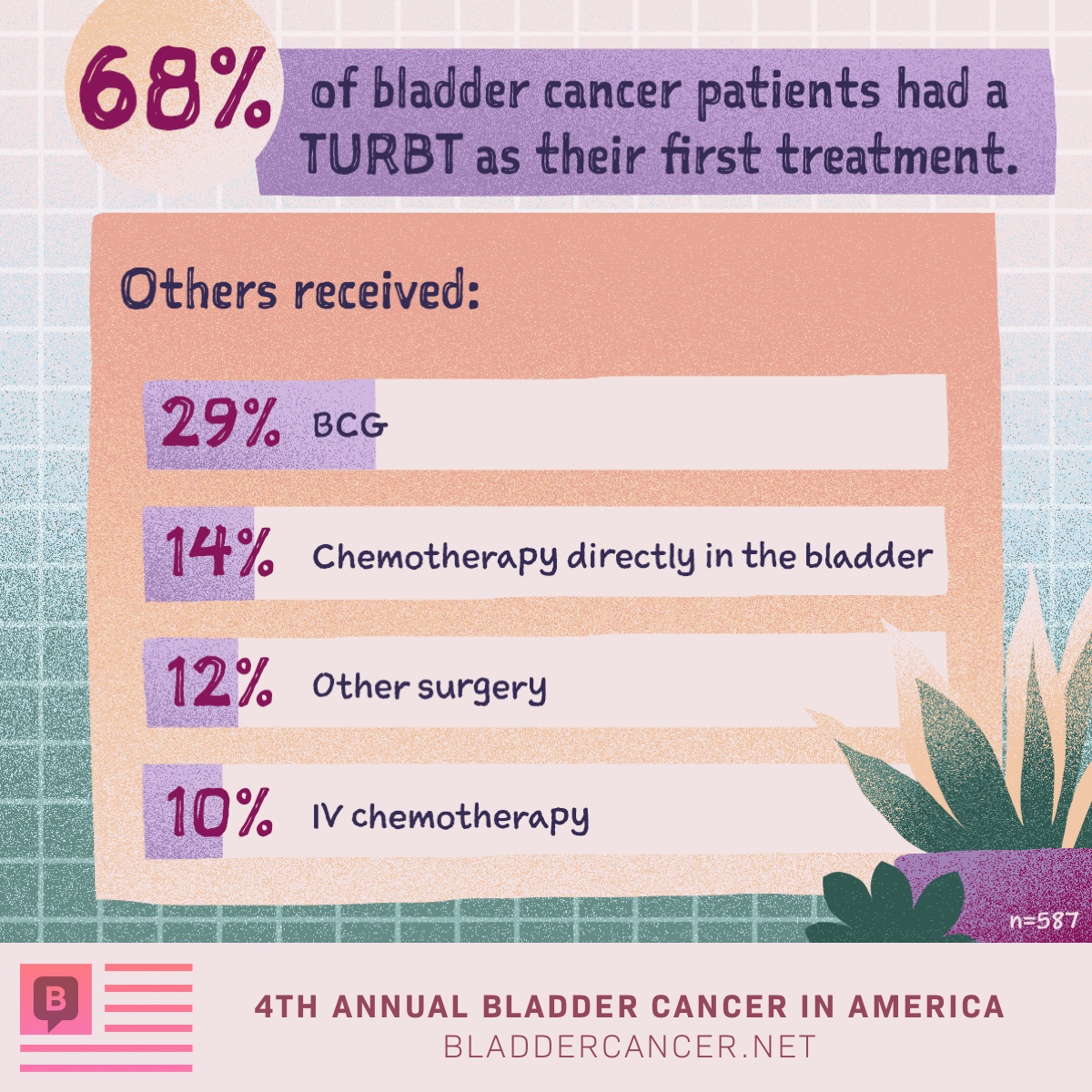
Non-muscle invasive bladder cancer treatments (NMIBC) In patients with NMIBC, tumors are confined to the inner cell layer of the bladder and have not invaded the thick muscle tissue of the bladder. NMIBC is usually treated by surgical excision in a procedure known as trans urethral resection of bladder tumor (TURBT), …
How is MIBC treated?
A far more threatening form of bladder cancer, MIBC is often treated by partial or complete removal of the bladder, usually after pre-surgery (neoadjuvant) chemotherapy, sometimes with concurrent radiation. After the tumor (or bladder) excision (adjuvant), more chemotherapy may be given.
What is the name of the drug that is used to treat PD-L1?
Another immune checkpoint drug, durvalumab (an anti- PD-L1 drug, brand name Imfinzi), combined with olaparib (a PARP1 inhibitor, brand name Lynparza) in a small trial produced complete pathologic responses in 50% of patients prior to tumor resection.

Is atezolizumab FDA approved?
It is worth noting that while the drugs atezolizumab and pembrolizumab were previously FDA-approved as first-line treatments for metastatic bladder cancer, both were later shown to have some benefit only in patients with PD-L1 positive cancers, and the label was modified accordingly, limiting availability of these two immune drugs to a smaller number of patients.
Is atezolizumab a first line treatment?
The combination of atezolizumab with chemotherapy as a first-line treatment has also produced promising results, but a combination of two immune drugs—durvalumab and tremelimumab— has failed in comparison to chemotherapy alone.
What is the best treatment for bladder cancer?
The most common bladder cancer drug that is given in early stage tumors is Bacillus Calmette-Guerin or BCG. BCG is a type of immunotherapy that ‘switches on’ the immune system which directs immune cells to the bladder. BCG treatment for bladder cancer is given after surgery to help prevent the cancer from coming back. 2,3

Where is bladder cancer found?
Bladder cancer – or urothelial cancer – is a common type of cancer. It most often begins in the cells that line the inside of the bladder, called urothelial cells. Urothelial cells are also found in other parts of the urinary system, such as the kidneys and the ureters. Urothelial cancer is found much more often in the bladder than in the other parts. But because people sometimes have tumors in these places, too, all of the urinary tract needs to be checked for tumors. 1
What is the most common symptom of bladder cancer?
The most common symptom of bladder cancer is blood in urine, which is usually painless. 1
What is targeted therapy?
Targeted therapy is a new type of therapy for patients with advanced cancer whose disease has progressed on chemotherapy and immunotherapy. One class of targeted therapies are antibody-drug conjugates (ADC), which can target and kill cancer cells while sparing healthy cells. ADCs are made up of 3 parts: 4
What is the purpose of chemotherapy?
Chemotherapy throughout body, to increase the chance for a cure in a person having surgery to remove the bladder, or as a primary treatment when surgery isn’t an option
Can bladder cancer be cured?
The prognosis of bladder cancer depends on various factors. Bladder cancer in the early stages (when it is confined to the lining of the bladder or when it has not spread to other places in the body) can often be cured. There is a change of recurrence, even with early-stage tumors, so treatment or surgery regular checkups are necessary. 2,3
Can you access bladder cancer drugs outside of your country of residence?
If you are trying to access new Bladder Cancer drugs that are approved outside of your country of residence, we might be able to help you access it with the support of your treating doctor. You can read more about the medicines we can help you and your doctor access and about their price below:

Abstract
Introduction: Bladder cancer carries a high healthcare burden and a poor prognosis once distant metastatic spread has occurred.
MeSH terms
Antineoplastic Combined Chemotherapy Protocols / administration & dosage
What is the FDA approved drug for bladder cancer?
Pembrolizumab is a FDA approved drug used to treat bladder cancer, head and neck cancer, Hodgkin lymphoma, lung cancer, and melanoma. According to the FDA, efficacy was investigated in KEYNOTE-057 (NCT, a multicenter, single-arm trial that enrolled 148 patients with high-risk NMIBC, 96 of whom had BCG-unresponsive CIS with or without papillary …

How many people have bladder cancer?
More than 61,000 men and 18,000 women are diagnosed with bladder cancer each year in the United States. Most of these men and women are over 70 years of age. Bladder tumors can be benign or malignant. Benign tumors are not cancerous and are not life threatening.
What is the name of the drug that is used to treat urothelial cancer?
On April 15, 2020, the U.S. The Food and Drug Administration also approved Jelmyto (mitomycin gel), the first therapy to treat low-grade upper tract urothelial cancer (UTUC). Urothelial cancer is a cancer of the lining of the urinary system.
When was Pembrolizumab approved?
On January 8, 2020, the Food and Drug Administration approved Pembrolizumab for the treatment of patients with Bacillus Calmette-Guerin (BCG)-unresponsive, high-risk, non-muscle invasive bladder cancer (NMIBC) with carcinoma in situ (CIS) with or without papillary tumors who are ineligible for or have elected not to undergo cystectomy.

Can doctors explain bladder cancer?
While doctors can’t explain why bladder cancer occurs, they have identified some risk factors.
Can bladder cancer recur?
They don’t invade tissue around them and once treated or removed, usually do not return. Malignant tumors are cancerous and have a high rate of recurrence. Bladder cancer can present with a variety of symptoms. Some of these symptoms are: Blood in the urine and urgent need to urinate or having to urinate more often.
Can DNA repair disrupt tumors?
Researchers know that DNA repair disruptions, although they may promote cancerous growth, can also make tumors highly susceptible to certain types of treatment. Thus, in principle, the researchers say, whole-exome sequencing of urothelial patients’ normal cells as well as tumor cells might allow many patients to be treated much more effectively.

Is bladder cancer an anatomical organ?
Representation of metastatic bladder cancer as an anatomical organ with malignant cells spreading in the human body. Credit: Shutterstock
Is bladder cancer inherited?
Although men are about three times more likely than women to get bladder cancers, and there are also specific environmental risk factors including smoking and exposure to industrial chemicals, studies of twins have suggested that the chance of getting bladder or other urothelial cancers is inherited. Yet relatively little has been known about the genes underlying that heritable risk, in part because prior studies in this field have tended to examine only limited sets of suspected risk genes.
Is urothelial cancer understudied?
Urothelial cancers and their genetic roots traditionally have been understudied, and treatments for these cancers are limited. The discoveries in the new study, published Dec. 3 in Nature Communications, could enable more targeted and effective treatments for patients who have these cancers.
Do urothelial cancers have inherited genes?
A significant percentage of patients with urothelial cancers have inherited gene variants that drive the progression of these cancers, according to a study from researchers at Weill Cornell Medicine and NewYork-Presbyterian. Urothelial cancers and their genetic roots traditionally have been understudied, and treatments for these cancers are limited.
Do urothelial cancer patients harbor germline variants?
In collaboration with Dr. Wendy K. Chung ’s team at Columbia University Vagelos College of Physicians and Surgeons, the authors found that these urothelial cancer patients are more likely to harbor this set of germline variants compared to non-cancer subjects.